In a recent post I wrote about my motivation to change my eating habits into a more vegan diet. But how does that go along with my running performance. In the interview with Fredrika Gullfot, who is just not only a vegan but also an Algae omega-3 supplement producer, I learned that her company produces omega-3 supplements for athletes.
So, you have probably heard, or read on labels of food about omega-3 but I must admit that 2 years ago, before I started to get into the details of nutrition, the name omega-3 was a bit confusing to me. However, omega-3 refers to the chemical configuration of an essential fatty acid and this super molecule appears to have many health benefits, being able to reduce inflammation, lower blood pressure, decrease risk of coronary artery disease and stroke and help protect against irregular heartbeats. Yes, it really sounds like a super molecule.
But what exactly is omega-3? My first question to answer in this article is how this super molecule function in our body? Second question, do I as a recreational-to-competitive runner need to supplement with extra omega-3? Is it really worth it, concerning its rather high price?
THE ESSENTIAL FATTY ACIDS OMEGA-3 AND OMEGA-6
Fat is an absolute necessity for life. The membranes that surround our body’s cells are predominantly composed of fat (lipids), and the brain is nearly 60 percent fat. The most common way to categorize fats is according to their degree of “saturation”. As seen on food labels, they are dived into saturated and unsaturated fats, with unsaturated fats further divided into monounsaturated and polyunsaturated. All three types are essential to our health.
Saturated fats serve a variety of critical biologic functions such as protein activation, maintenance of cell membrane rigidity, and induction of apoptosis (programmed cell death) in cancer cells. However, saturated fats have been demonized in recent years. As saturated fats are typically solid at room- as well at body temperature, logic would suggest that saturated fats are the “artery clogging” agents of cardiovascular disease and therefore should be avoided (I will discuss this more later).
Unsaturated fats has the presence of “double-bonds” in their molecular structure. This gives these molecules a degree of flexibility or firmness. These molecules are therefore oils at room temperature unlike saturated fats, which are predominantly solid. Also the presence of the double bond in unsaturated fats gives them a degree of reactivity.
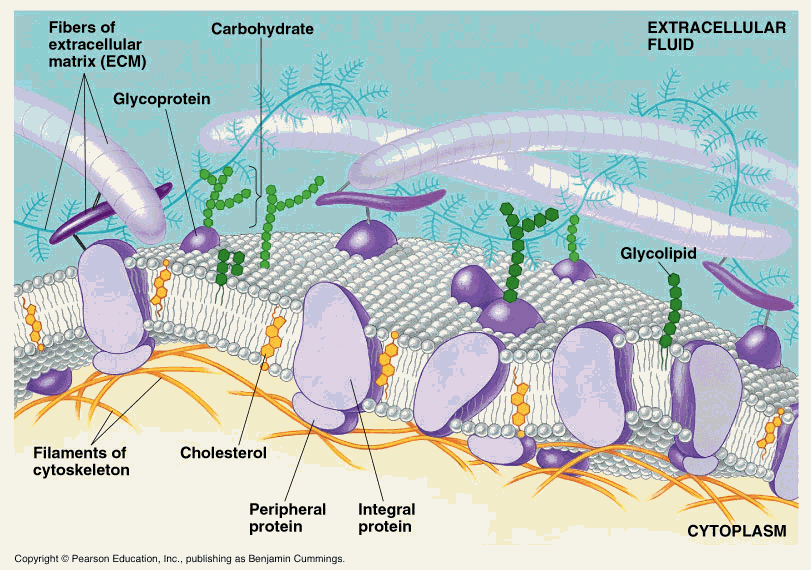
Between the years 1929 to 1978, the two essential polyunsaturated fatty acid (PUFA) classes’ omega-3 and omega-6 were defined. If these PUFAs are not sufficient in our diet over months (omega-6) or over decades (omega-3), then bodily dysfunction occur and we are prone to disease. Both classes serve structural functions, constituting cell membranes/lipid layers in many different cells throughout our body, as well as having roles in cell-cell signaling (Figure 1). Through a series of enzymatic reactions, these fatty acid substrates are converted to chemical signaling molecules, the so-called “eicosanoids” (Figure 2). Those derived from omega-6 fatty acids are so called pro-inflammatory, as they can induce bodily inflammation, while those from omega-3 fatty acids possess more anti-inflammatory properties. The omega-3 and omega-6 fatty acids are both essential to life but their relative dietary intake ratio is important, where an omega-6:omega-3 ratio of 1:1 is optimal for life-long health.
Figure 1: Illustrates a membrane surrounding a cell. Fatty acids with various chemical configurations are forming a lipid layer. Transport- and signaling proteins span this cell membrane, facilitating transport of nutrients and signaling molecules from the cytoplasm to the extracellular matrix. Picture courtesy and copyright: Pearson Education.
Omega-3 fatty acids are highly concentrated in the brain and have been shown to be important for cognitive (brain memory and performance) and behavioral function. The integration of the omega-3 fatty acids, into the brain is critical for development during fetal and post-natal periods. Infants who do not get enough omega-3 fatty acids from their mothers during pregnancy have higher risk for developing vision and nerve problems. Myelin, the encapsulating material that serves as “insulation for the nerves”, is composed of the omega-3 fatty acid DHA. In diseases such as multiple sclerosis, categorized as a “demyelinating” disease, the body attacks this myelin sheath via an autoimmune process and insulation is lost. Nerve impulses cannot longer be controlled. Symptoms of omega-3 fatty acid deficiency include fatigue, poor memory, dry skin, heart problems, mood swings or depression, and poor circulation. Along with omega-3 fatty acids, omega-6 fatty acids also play a crucial role in brain function, and for normal growth and development. Deficiency of omega-6 has been shown to cause skin rash, growth stunting and sterility.
Biochemical pathways for production of the essential omega-3 and omega-6 fatty acids
Our bodies can make most of the fatty acids we need, but the two types of essential PUFAs; linoleic acid (LA) and alpha-linoleic acid (ALA), we have to obtain from our diet.
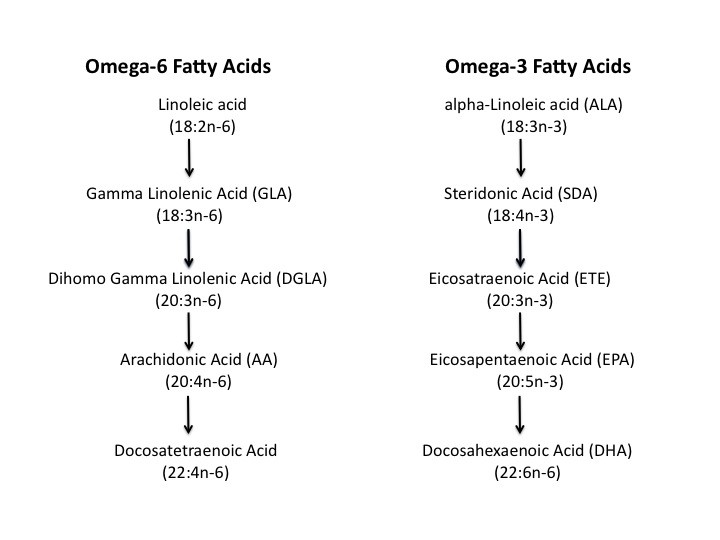
Linoleic acid (LA) is an omega-6 fatty acid constituted by 18 carbons atoms, 2 double bonds, with the last double bond sitting 6 carbon atoms from the omega-end (18:2n-6). Alpha-linoleic acid (ALA) is an omega-3 fatty acid constituted by 18 carbons atoms, 3 double bonds, and with the last double bond sitting 3 carbon atoms from the omega-end (18:3n-3) (Figure 2).
Figure 2: Illustrates the biochemical pathways for transformation of the polyunsaturated fatty acids linoleic acid (LA) and alpha-linoleic acid (ALA) to highly unsaturated fatty acids. The omega-3 ALA is a precursor for production of the essential EPA and DHA, which are highly unsaturated fatty acids containing 5 and 6 double bonds.
The important roles of the omega-3 Fatty acids EPA and DHA
The human body can convert the alpha-linoleic acid (ALA) found in vegetables sources such as walnuts, flax seeds and soy into the omega-3 FAs eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), but our body is not very efficient in doing this. With the low conversion of ALA to DHA in humans it means that our DHA demand is not met. However, when our body is provided with DHA directly via the diet we can use DHA as a precursor to produce all the other essential forms of omega-3s, since the omega-3 pathway in Figure 2 is reversible.
Cold-water fish and cold-adapted mammals contains the omega-3 FAs EPA and DHA in high amounts. The fishes also obtain their ALA from vegetables sources inform of microalgae. However, cold-water fishes are much more efficient in transforming ALA into EPA and DHA, where these longer, more bent, and flexible fatty acid molecules keep the cell membranes from becoming too stiff when exposed to very cold to freezing conditions.
The high amounts of DHA in fish is the main reason why researchers and doctors began to recommend us obtaining our DHA directly, from fish or fish oil. Since DHA was shown to be the active component for lowering triglycerides in our blood, and for bioavailability to the brain and organs, cardiologists began recommending their patients to take 1 gram per day of combined EPA/DHA. Studies claim that with no major diet changes, improvement of blood DHA status can be achieved with dietary supplements of preformed DHA, but not with supplements of ALA, EPA, or the other precursors (Figure 2).
To maintain health we need to balance our omega-6 to omega-3 intake
As mentioned before the ratio of our intake of omega-6 to omega-3 is important for our health. Also the actual requirement for these two forms is low, where about circa 1% of our daily energy should come from each of these classes. However, a lot of Europeans and Americans consume about ten times the amount of omega-6 they need due to frequent intake of soy, corn, cottonseed, peanut, sunflower, and safflower oils. By contrast, few barely meet the minimum 1% for omega-3 (Volek and Phinney, 2012). Hence, when the ratio and the concentrations of these fatty acids are wrong the equilibrations of the biochemical reactions are shifted and the specificity of enzymes change. We cannot build cell layers with the right conformations and functions, and cell-cell signaling is impaired.
Both omega-3 and omega-6 fatty acids are incorporated into cellular membranes as phospholipids. And while small amounts of omega-6 fatty acids are essential to the body, high concentrations within the cell membrane from excess consumption are casually related to bodily inflammation and more specifically, chronic disease. For example, the increase in arachidonic acid AA (an omega-6 fatty acid derived from the metabolite DGLA, see Figure 2) has been shown to lead to an increase in pro-inflammatory prostaglandins, and to a decrease in phospholipids derived from EPA/DHA (omega-3 fatty acids). When the omega-6:omega-3 ratio of the cellular membrane is increased due to the surplus of omega-6 fatty acids in the European/American diet, we become more susceptible to disease, especially. Systematic bodily inflammation over long-term makes us susceptible to a whole host of chronic and age-related diseases, where the most common of which is cardiovascular disease (Osborn, 2014).
Why do we eat the fats the way we do?
In the book “The Art and Science of Low Carbohydrate Living” by Jeff Volek and Stephen Phinney they dedicate one chapter about why we today eat the different dietary fats we do. They explain that hunting cultures learned to time the hunt to obtain optimum fat content of their kill. They also learned to hunt for fats. For example, on the North Pacific Coast, sea lions and seals were harpooned for food and skins. Even though these animals were rich in fat, the people of this region chose to focus on catching and processing the tiny oolichan as their primary fat source. Why? Today we know that oolichan grease and seal oil have different chemical and physical properties. Seal oil is rich in omega-3 fats, and promptly goes rancid upon exposure to air, whereas oolichan grease, is low in polyunsaturated fatty acids, and mostly consists of monounsaturated and saturated fatty acids. The oolichan grease is therefore more stable in storage, allowing it to be kept for a year or more without going bad. (Umm… How should we eat our omega-3 rich foods? Should we preferably eat our salmon and tuna raw? Does smoked salmon have intact omega-3 fat that our body can use? )
EXERCISE, ROS AND HUFA
What happens during exercise and what is recovery?
The body’s response to exercise is fascinating and complex. When we exercise intensely, we damage tissues at the microlevel, which causes an acute-inflammation. Our body needs inflammation, but for discrete periods of time only, to fend off disease, repair tissue – for example a muscle injured during a workout. So after a workout, the body’s reparation system is put into work upon stimuli from inflammatory signal molecules and this reparation cascade is what ultimately makes us stronger, leaner, fitter, and more muscular. However, long-term and chronic inflammation is a primer for chronic disease. This is foundational, and paramount to our understanding of aging and age-related disease. Every disease possesses an underlying inflammatory component, so if we want retard our aging we should minimize long-term inflammatory processes (Osborn, 2012).
Adaptation and recovery from exercise can be studied by measuring various metabolites, hormones, membrane components, inflammatory signals, immune cells, and markers of oxidative stress and muscle damage. ROS (reactive oxygen species) are metabolites tightly linked to inflammation. Exercise increases ROS production. This is because a small fraction (1-3%) of the oxygen we use in our mitochondria, to produce energy to fuel running or other muscular movement, generates ROS. Most of the ROS are captured and quenched by our anti-oxidant system such as superoxide dismutase (SOD), glutathione, and tocopherols (vitamin E), but some of the ROS escape this defense system. So, the more we use, and the greater demand we put on our metabolic system (i.e our mitochondria), the higher volume of ROS production.
Studies of athletes engaged in prolonged intense exercise has shown that even in highly trained athletes the anti-oxidant defense system can be overwhelmed, with leaky ROS attacking cell membranes, and especially the highly unsaturated fatty acids (HUFA). This ROS-mediated destruction of HUFA in membranes can have an overall deleterious effect on recovery from exercise by impacting metabolic, inflammatory, immune, coagulation and fibrinolytic processes (see chapter 5 in Volek and Phinney (2012) and references therein). Understanding how to protect and counteract ROS is important for optimizing recovery after high volume training or competition.
Insulin Sensitivity – Link between Alaskan sled dogs and Marathon Runners?
It is widely accepted that exercise improves the insulin sensitivity of muscle cells, and seen as a group, highly trained endurance athletes tend to be very insulin sensitive. During the 1990’s, a Finnish research group studied insulin sensitivity and muscle glycogen recovery in a group of runners completing a marathon. This group discovered that the runners were more insulin resistant in the first few days after the marathon than they were before the race, and this occurred despite their muscles still being mostly empty of glycogen (Tuominen et al., 1996). (Umm…what does it really mean to be insulin sensitive or insulin resistance?)
Insulin sensitivity is a term used to describe how well a tissue responds to the hormone insulin when it comes to processing glucose, the sugar transported with our blood. The pancreas is responsible for secreting insulin and this hormone is secreted upon a rise in blood sugar. Insulin then triggers tissues in the body, mainly skeletal muscles and livers cells, to absorb glucose from the blood and store the glucose in form of glycogen. Consequently, when glucose is withdrawn from the blood into the muscles, then blood glucose level is lowered back to normal range (70-80 mg/dL). In someone with insulin sensitivity, very small amounts of insulin is required for the tissues to respond by absorbing glucose. In someone with insulin resistance, large amounts of insulin are needed to achieve the same effect.
So, back to the marathon runners. When their body is expected to be most insulin sensitive and in most need to rapidly rebuild its glycogen reserves, their post-marathon bodies appears to have run into a temporary metabolic roadblock. This observation, called the ‘post-marathon paradox, has also been confirmed by another scientific group (Asp, et al., 1997), but still not been fully explained. So, let us look into if we can learn something from dogs.
Super Endurance Athletes – Alaskan Racing Sled Dogs
Alaskan sled dogs are elite endurance athletes, capable of running 250 to 300 km per day at a pace of 15–20 km per hour in extreme conditions over many consecutive days. Racing sled dogs have a remarkably high sustained metabolic rate during competition, and their energy expenditure during these races can be as high as 11 950 Kcal per day!!! To meet energy demand and to reduce musculoskeletal injury, sled dogs usually are fed a diet high in fat (> 50% of energy content) and protein (> 25%), but low in carbohydrate (< 20%).
During the 1000-Mile Iditarod race, where the dogs pull their sleds more than 160 kilometers per day for 8-10 consecutive days, a scientific study was performed looking into different metabolic factors such as glycogen and fat usage, and markers of oxidative stress and muscle damage. The hypothesis was that the cumulative oxidative stress in these dogs would degrade membrane phospholipids essential fatty acids (MP-EFA), and that this effect over 10 days would be better observed in cheek cells (with fast cell turnover) compared to red blood cells (with slow cell turnover). Researchers took blood and check swabs from a small number of dogs from three different teams before and after the 1000-Miles competition. It turned out to be a considerable difference in observed changes within the membranes between the three racing teams. There was little change in red blood cell MP-EFA, however all teams showed numerical reductions in one or more classes of cheek cell MP-EFA. In one team, the reductions in both omega-3 and omega-6 MP-EFA classes were greater than 50%. A second team demonstrated intermediate changes, and one team had little to no changes. The conclusion was that the gut membranes (i.e., cheek cells) were subject to dramatic alternations due to oxidative stress from prolonged exercise. Even though the exact diet compositions for each different team was unknown, the significant differences in MP-EFA content strongly suggest that diet plays a major part in moderating this effect. (Umm…Maybe the dogs in the different teams were fed with different dietary fat sources?)
The concentration of MP-EFA is related to insulin sensitivity and insulin resistance
Some of the most vulnerable molecules in cellular membranes nearby for ROS attack are the membrane phospholipids AA, EPA and DHA (Figure 2). The omega-6 arachidonic acid AA is tightly linked with insulin sensitivity; and because it is the dominant fatty acid in the membranes of human muscle cells, it also is the target for ROS, where even a 25% reduction in muscle MP-EFA dramatically reduce insulin sensitivity (Borkman et al., 1993). Volek and Phinney have performed studies on how membranes and especially MP-EFA are damaged by ROS during prolonged exercise. They suggest that their experimental set-up, where cheek cell swabs from the over-exercised athlete are withdrawn and analyzed on their AA content, could be a valid measure of exercise-induced membrane damage. It provides a test of the athlete’s oxidative stress status and its risk of over-training.
HOW TO BUILD STRONGER MEMBRANES AND PROTECT THEM AGAINST ROS DESTRUCTION?
For our cells to work properly, and especially our muscle cells which we use during running, we have to find ways to maintain our cellular membranes in good shape. In the first place we can build strong cellular membranes by having the right balance of omega-3 and omega-6 derived MP-EFAs within them (Figure 2). Second, we can try to minimize oxidative stress from ROS which will lead to less destruction of the membrane (less holes to be repaired, hence less inflammation). The dream situation is to only stimulate the cellular repair machinery after a given workout – referred to exercise adaptation.
So, how do we provide our body with the right omega-3 to omega-6 balance? And how do we minimize oxidative stress from ROS so that these are mainly caused by exercise?
To answer these questions I will turn to the experts!
“Maintaining adequate membrane MP-EFA status can be further supported by ensuring adequate intake via your diet or via supplements of omega-3 and antioxidant/anti-inflammatory compounds like the ‘gamma form’ of vitamin E. Omega-3 supplements would be of higher importance for athletes thriving of a vegan diet” – Volek and Phinney, 2012
“Create a favorable internal environment through sound nutrition, by limiting refined sugars and increasing consumption of both dietary fiber and omega-3 fatty acids” – Dr. Brett Osborn, 2014
Eat more omega-3 rich food and avoid food rich in omega-6 rich
Be picky about your fats. Think of the essential fat classes omega-3 and omega-6 as if they are fat soluble vitamins. Remember that only about circa 1% of our daily energy should come from each of these classes.
To build better cell membranes, to defense our self towards ROS, and the risk for chronic inflammation and disease, we should increase our dietary omega-3s. Vegetable sources such as flax, hemp, chia, and green leafy vegetables (kale and spinach), provide us with ALA. Fish, fish oils and algae oils provides us with EPA/DHA. We should also try to avoid omega-6 rich vegetable oils such as the ones already mentioned above (soy, corn, cottonseed, peanut, sunflower, and safflower oils). The goal is to get closer to a ratio of 2:1 or 3:1 of omega-6 to omega-3 from the current 10:1 to 20:1. Omega-6 has in the past been encouraged as a substitute for animal fat. Vegetable oils such as corn oil, sunflower, safflower, soybean, and cottonseed oil, as well as margarine were touted by public health authorities as “heart healthy”. However, data suggests otherwise. The Sydney Diet Heart Study with 458 participants demonstrated that substitution of dietary linoleic acid (LA) (precursor in omega-6 pathway, Figure 2) in place of saturated fats increased the rates of death from all causes, coronary heart disease, and cardiovascular disease (Ramsden et al., 2013).
Also, our metabolism of omega-3 to omega-6 fatty acids is claimed to be profoundly changed if we restrict our body of simple high-glycemic carbohydrates. Volek and Phinney has demonstrated in both human and animal studies that keeping a diet where simple carbohydrates with high glycemic index are excluded associated with increased levels of AA and DHA in blood phospholipids and tissue membranes. The body makes more efficient use of both classes of essential fats compared to when fed a high carb diet, but without signs of an increase in production, suggesting that their rate of degradation goes down when dietary carbohydrates are limited (Umm… Less glucose to burn, less use of mitochondria, less ROS and therefore less oxidative stress…?)
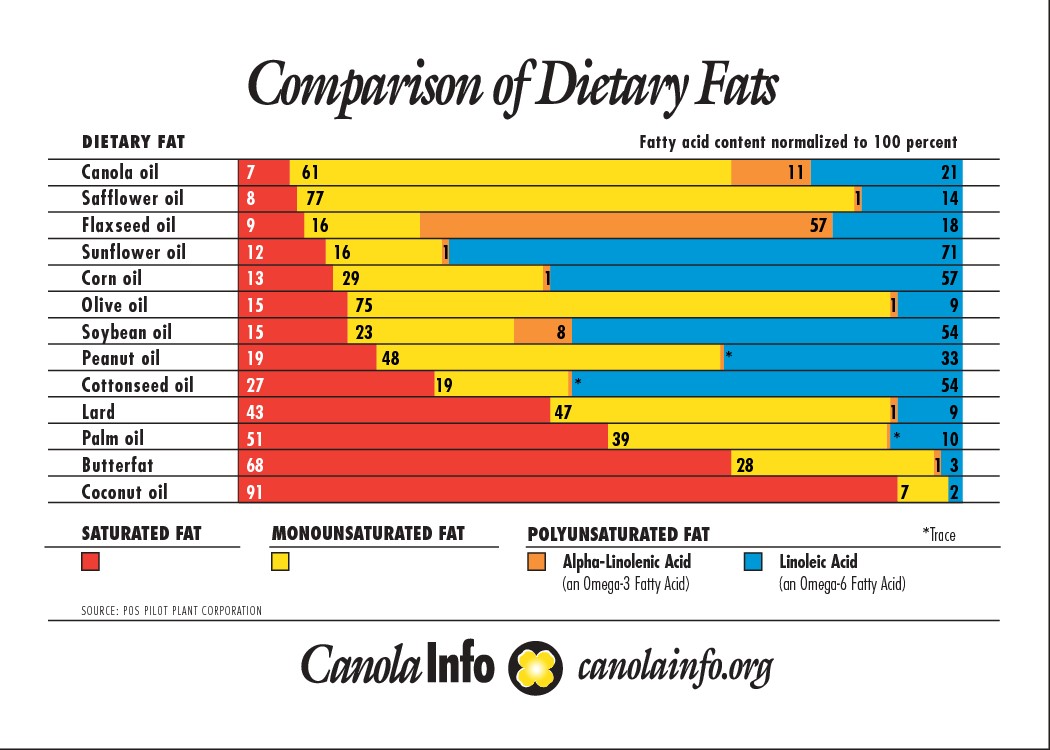
So, when we dear to eat a diet higher in fat there will be so much omega-6 fat in our food supply that it is unlikely that we come up short. As for the omega-3s, Volek and Phinney recommends that we eat either 3 fish meals per week or supplement with 1 gram of fish oil daily. They also recommends that we give high priority to mono-saturates, then saturates, and make reasonable efforts to avoid foods rich in omega-6. When possible, we should avoid mayonnaise, and salad dressings made with oils rich in omega-6 such as soybean, corn, sunflower and cotton seed oils (see Figure 3 below for detailed fatty acid content in different dietary fats).
Figure 3. Illustrates the relative percentage of different fatty acids (saturated, monounsaturated, and polyunsaturated (omega-3 ALA and omega-6 AL forms) in various common dietary fat sources.
Did you know, that a 50:50 mixture of butter and olive oil approximates the composition of triglycerides typically found in human body fat?
There are additional reasons why athletes may benefit from reducing their omega-6 to omega-3 consumption. As mentioned above omega-6 fats are more strongly associated with inflammation than omega-3 fats. Increasing the omega-3 status consistently leads to lower levels of inflammation, and it also has a potent effect on lowering fat levels (triglycerides) in the blood. In addition to being linked to many chronic disease states, chronic elevations in inflammation can impair recovery from exercise, compromise adaptations to training, and increase the risk of injury. Also, peak aerobic power, VO2max, has been shown to be negatively associated with biomarkers of inflammation, like interleukin-6 and C-reactive protein. Reducing systemic bodily inflammation would then facilitate cellular energy metabolism, hence increase endurance and performance (Volek and Phinney, 2012).
Though I am fueling my running on a fairly high-fat-low-carbohydrate diet, and know that I am rather insulin sensitive, I do not eat the amounts of fish recommended to fulfill my daily requirements of omega-3. As I train every day, and I will keep on doing this during this year, I believe my running performance (as well as my dry skinned hands and feet) could benefit from me supplementing my diet with more omega-3.
OMEGA-3 FOODS AND SUPPLEMENTS
As mentioned in the introduction, we humans cannot create EPA and DHA very efficient from the ALA precursor found in green leafy vegetables, nuts and seeds. EPA and DHA are often cited as being the beneficial components of fish oil, yet they actually originate from microalgae. Marine algae are one of the most abundant organisms around and they are the base of the food chain for fish. Via photosynthesis, microalgae harness energy from the sun, and convert carbon dioxide into biomass (proteins, carbohydrates, fats) and oxygen. In essence, algae have three components that make them nourishing both for us and fishes to eat: chlorophyll and other plant pigments; omega-3 fatty acids in the form EPA and DHA; and important marine minerals such as iodine. When fish consume algae they are as mentioned before are able to transform the ALA into EPA, and the EPA into DHA, as well as to concentrate these forms in high amounts in their cellular membranes and tissues.
Why Algae Oils?
From the interview with Fredrika Gullfot I learned that some of the cultivated fish that we buy as our omega-3 supply might not have the amounts of omega-3 we are looking for. If the fish has not been feed with algae, but with yeast or soy, they do no concentrate high amounts of EPA and DHA and they are therefore a poor omega-3 source. Therefore we should buy wild-caught fishes, which are higher in omega-3. There is only one problem: the fish stock is not endless and not sufficient. Fish oil and fish meal account for by far the biggest catch of the oceans, in terms of volume. Fish oil is the raw commodity for approximately 95 percent of all omega-3 EPA & DHA sold in the world, a rapidly growing market for food, dietary supplements, pharmaceuticals and pet food. Between 2011 and 2016, it is estimated that the ingredient market for omega-3 EPA & DHA will increase by almost 50%. The large-scale trawling for fish oil and fish meal also creates serious environmental problems due to overfishing and irreversibly destroyed coral reefs. According to reports from the United Nations Fisheries and Agriculture Organization, global fish stocks might collapse in 2048, if the devastation of the oceans continues at the same rate as today. (source Simris, a Swedish algae oil producer (www.simrisalg.se)).
Since it apparently takes 600 sardines, to produce one bottle of omega-3 fish oil supplement (ca 60 capsules), it sounds much more environmentally friendly to go straight to the source, and rather produce omega-3 oil from algae. Algae, similar to plants, can be grown in greenhouses, but in closed systems called photobioreactors. These are designed so that algae are grown under controlled conditions and exposed to as much sunlight as possible, in order to optimize photosynthesis and growth. The closed environment ensures quality and purity, with an omega-3 oil that is ecologically sustainable and free from environmental toxins. Farmed algae-derived DHA is approved for infant formulas and can already be found in many applications, including fruit juices, milk, soy milk, cooking oil, sauces and tortilla (online article in FoodProcessing by Mark Anthony, 2012)
Recommendations on Daily Dosages from Different Nutritional and Medical Specialist
Dr. Osborn: Omega-3 Fatty are vital to your health and particularly beneficial to your heart and brain. Purchase purified omega-3 FA capsules, since not all are created equal, and some can be laden with omega-6 FA. Pay particular attention to the quantity of omega-3 per capsule and dose accordingly. Chose fish oil with the most omega-3 FA per capsule and the least omega-6. Your goal is to minimize intake of omega-6 FA and maximize omega-3 FA intake. To optimize your omega-6:omega-3 ratio, supplement with a minimum of 3 grams (3000 mg) daily, divided in smaller doses. Many individuals handle up to 10 to 15 grams daily without adverse effects, but at high dosages (> 3000 mg daily) potential interference with blood clotting. Bloating, belching, and diarrhea are common side effects of omega-3 supplements. Recommended is to simply store your capsules in the freezer; the fatty acids will then be released in a more delayed manner into the gut and these side effects diminished. Storing the fish oil in the freezer also slows down the oxidation process. (Umm…Meaning that we should eat our omega-3 food sources such as salmon and tuna raw!??)
Volek and Phinney: Claims that the minimum dose to start with is 500 mg of EPA plus DHA per day, which is equivalent to about one serving of fatty fish every other day. A more optimal dose for most people may be closer to 1 gram per day of EPA and DHA. If you are at risk of heart disease, stroke or inflammatory condition, they recommend 2 grams per day for better results. Claims that DHA derived from microalgae at a minimum dose of 200 mg per day is a viable option.
Good sources of omega-3 fatty acids are salmon, tuna, sardines, and herring. Ideally consume them 2-3 times per week. Another available alternative to eating fish or fish oil capsules is omega-3 eggs. These are produced by feeding hens a diet rich in omega-3 fats, resulting in 100-150 mg of EPA + DHA per egg. Thus two of these omega-3 eggs would suffice the minimum daily dose without the need to eat fish at all. The response to omega-3 rich foods or fish oil supplementation varies between individuals, some required higher doses to achieve the same physiological effects (see review article by Jeromson et al., (2015)). (Umm…Usually doses are calculated based on body weight with a general reference value of a man of 70-80 kg. I am a 50-kg woman and will suffice with a smaller daily dose.)
Precision Nutrition: Recommend that we supplement with algae oil or fish oil daily. They recommend 2 g of algae oil, or about 3-6 g of fish oil each day.
CONCLUSIONS
Omega-3 supplements as a recovery drink nutrient similar to protein and carbohydrate?
After long distance endurance events, and events that last consecutive days (like for example “Tour de France” for cyclists, or “Tour de Ski” for Cross-country skiers, it is not unusual that athletes faces the traits of an overwhelmed anti-oxidant system, catching a cold. Based on the data from the Alaskan sled dogs this cold could be due to an oxidative overstressed respiratory system. One could then speculate that a high quality omega-3 source would be beneficial in the recovery drink together with amino acids and carbohydrate.
In order for our bodies to use nutrients to rebuild and recover, those nutrients have to be available. And if they are available, then our body is more likely to use them. Simply having the materials around can be enough of signal to our body that it is time to rebuild.
Directly after exercise our blood is circulating more rapidly. We can improve the muscles nutrient availability by having more nutrients in that circulating blood, by providing nutrients immediate to the workout. The post-workout phenomenon referred to as “the window of opportunity” imply that our muscles are primed to accept nutrients that can stimulate muscle growth, muscle strength and muscle repair. This window opens immediately or even during the workout but closes relatively quickly. Research suggests that while protein synthesis persists for at least 48 hours after exercise, it is most important to get post-workout nutrition immediately up to maximum 2 hours afterwards.
My idea here is that it would be beneficial to add the omega-3 fatty acids, EPA and especially DHA, to the post-workout nutrition quite immediate after intensive and extensive races, or for example during intense weeks with many races, or differently put, at times when the metabolic machinery (the mitochondria) has been highly used together with extensive muscle cell damage. There is at the moment no specific recommendations to supplement with higher doses of omega-3 during events like “Tour de Ski” for cross-country skiers in the Swedish National Team (comment Cross-Country Skier, Maria Rydqvist).
Sustainable eating – shifting from animal-based to plant-based
I agree that we have evolved on a diet involving animal sources, but today we are faced with the problem that we much more human beings on this planet. The animal sources are limited. To survive as a species we might have accept a systemic change and find solutions to a more plant-based diet. Similar to our ancestors we have to find food sources that are sustainable but that gives us the essential nutrients that our body needs.
I am training and competing at a semi-professional level and from the things that I learned about the benefits of omega-3 it is clear to me that I would benefit from having more omega-3 in my diet. I want to start supplementing my diet with omega-3 not to be dependent on eating my share of fish every week. However, when I hunted for a good algae omega-3 supplement I found that a substantial part of the content in the capsules is just not EPA and DHA oils, but flaxseed and sunflower oils (Figure 4).
Figure 4: Illustrates the composition and content of an algae omega-3 supplement from supplier Dr. Fuhrman. Each capsule of contains not only the omega-3 oils EPA and DHA, but also sunflower oil which is rich in omega-6.
I could live with the flaxseed, but not with the sunflower oil. I have written many sentences above that we should aim at reducing our intake of omega-6 in favor of omega-3 to have the right balance for building strong and functional cell membranes. I asked Fredrika Gullfot at Simris to comment on the sunflower oil that I found in so many vegan algae omega-3 supplement. In Simris case the EPA and DHA are mixed primary with omega-3 rich flax seed oil but the DHA oil is not yet produced in house and therefore bought from another supplier. This supplier delivers its DHA mixed with sunflower oil. However, the amount should according to Fredrika be less than 10% and in the future Simris wants to produce smaller capsules that are sunflower oil free. Umm…Why just not mix the EPA and DHA oils with extra virgin olive oil? This oil contains mostly monounsaturated fatty acids that could be used for fuel running and olive oil does not oxidize as fast as for example flaxseed oil.
Until there is an algae omega-3 supplement without additional omega-6 rich vegetable oils, I will focus on getting my essential fats from whole foods such as nuts, seeds (flax and chia are especially nutritious and rich in the omega-3 ALA), fish, leafy green vegetables and eggs. Foods as they come in nature – not too refined, not too processed, and not too heated. This should ensure that my body is fueled with the right balance of nutrients and in the right concentrations (Figure 3 and Figure 5).
Figure 5: Illustrates the amounts of sunflower seed required to produce 80 mL of sunflower oil. We easily* ingest a serving of 10 – 15 mL of oil, whereas it is much more difficult to eat the respective amounts of seeds.
*Here I refer to Steve Phinney’s ketogenic diet experiments, where he fed on the omega-6 rich vegetable oils (soybean and corn) but felt prominent nausea and gastro-intestinal upset (chapter 8, Volek and Phinney (2012)).
REFERENCES AND FURTHER READING:
Jeff S. Volek, and Stephen D. Phinney, The art and science of low carbohydrate performance, (2012)
Dr. Brett Osborn, Get Serious, (2014)
http://www.precisionnutrition.com/all-about-fish-oil
http://www.precisionnutrition.com/all-about-algae
Mark Anthony, Ph.D., Technical Editor, Is Algae DHA As Healthy as Fish Oil DHA? – A review of research earlier this year found mostly good news in this vegetarian source. http://www.foodprocessing.com/articles/2012/May 22
Tuominen, J.A., Ebeling, P., Vuorinen-Markkola, H. and Koivisto, V.A. (1997), Post-marathon Paradox in IDDM: Unchanged Insulin Sensitivity in Spite of Glycogen Depletion. Diabet. Med., 14: 301–308.
Asp, S., Daugaard, J. R., Kristiansen, S., Kiens, B. and Richter, E. A. (1998), Exercise metabolism in human skeletal muscle exposed to prior eccentric exercise. The Journal of Physiology, 509: 305–313.
Ramsden, C., Zamora D., Leelarthaepin B., Majchrzak-Hong S., Faurot K., Suchindran C. et al., (2013) Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis. BMJ, 346:e8707
Forsythe, C.E., et al., (2008) Comparison of low fat and low carbohydrate diets on circulating fatty acid composition and markers of inflammation. Lipids, 43(1):p. 65-77
Borkman, M.; Storlien, L.H.; Pan, D.A.; Jenkins, A.B.; Chisholm, D.J.; Campbell, L.V. (1993) The relation between insulin sensitivity and the fatty-acid composition of skeletal-muscle phospholipids. N. Engl. J. Med., 328, 238–244.
Stewart Jeromson, Iain Gallagher, Stuart Galloway, D. Hamilton. (2015) Omega-3 Fatty Acids and Skeletal Muscle Health. Marine Drugs 13, 6977-7004